We are a “One-Stop” centrally located (near QEW & Niagara St.) foot clinic in St. Catharines offering quality custom orthotics and comprehensive chiropody / podiatry services including:
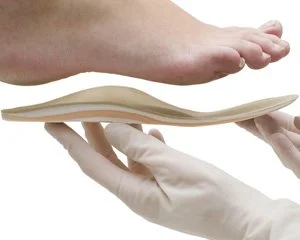
CUSTOM ORTHOTICS (using 3D digital casting: highly accurate & comfortable made at an accredited Canadian laboratory). Niagara’s first clinic to offer this leading technology. Learn more
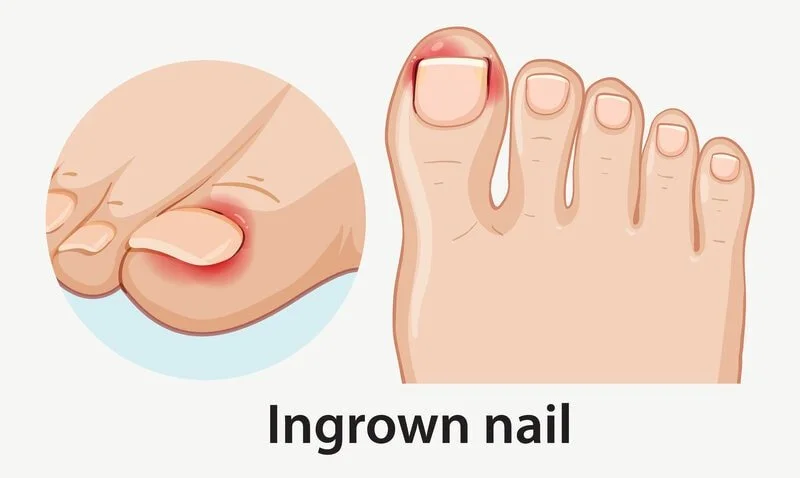
INGROWN TOENAIL CORRECTION procedures using minimally invasive surgery & non-surgical techniques for your comfort. Learn more
FUNGAL TOENAIL LUNULA LASER & a variety of topical treatments. Learn more
FOOT WART SWIFT Microwave Technology & Liquid Nitrogen wart freezing treatments. Learn more
HEEL PAIN RELIEF & Plantar fasciitis treatments. Learn more
FOOT PAIN treatments for ball of foot pain, flat feet and more. Learn more
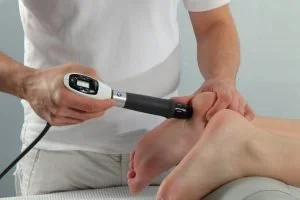
SHOCKWAVE THERAPY to accelerate soft tissue healing of conditions such as plantar fasciitis and Achilles tendonitis. Learn more
FOOT CARE (Medical Pedicures) for corns, calluses and toenails. Learn more
DIABETIC FOOT CARE: Examination and monitoring of diabetic foot health. Diabetic Medical Pedicures for corns, calluses & toenails. Learn more
Orthopedic FOOTWEAR: offering an attractive selection of modern styles from leading manufacturers to fit your lifestyle and relieve foot pain. Learn more
Whether you are seeking heel pain relief , clear toenails for summer, wart-free feet or foot pain treatment options, we offer a range of effective treatment options to suit your lifestyle.